The Stress-Immunity Feedback Loop
Compound evidence detail1 SCR / 2 parts
- Documentedthe canine telomere-shortening evidence under documented chronic stressors such as kenneling, shelter conditions, low activity, and large group housing (Dutra 2025, N=250)
- Heuristicthe JB extrapolation that chronic household excitability produces equivalent telomere shortening to documented institutional stressors and reduces canine lifespan
Chronic stress does not stay politely confined to mood or behavior. In dogs, it can alter immune-related function, shift mucosal defense markers, and in more adverse long-term contexts even track with shorter telomeres, which is why JB treats stress as part of a feedback loop between body and behavior rather than as a purely emotional problem. Heuristic
What It Means
The first half of the loop runs from stress into the body. Chronic adverse stress changes endocrine signaling, immune-cell behavior, and recovery processes. Documented The strongest direct dog evidence comes from sheltering, restriction, kennel stress, and other more severe long-duration contexts, not from ordinary lively households. That boundary matters and should stay visible.
The second half of the loop runs back from the body into behavior. A dog whose immune system is taxed, whose gastrointestinal system is irritated, or whose physical resources are under strain is less behaviorally resilient. Documented Illness increases discomfort, reduces tolerance, interrupts sleep, and makes recovery harder. That means stress can worsen physical vulnerability, and physical vulnerability can then worsen stress expression.
Mucosal-immune research adds a useful layer. Documented In dogs, salivary cortisol correlates negatively with salivary secretory IgA, and delayed recovery of that marker after stress is associated with more fearful and anxious phenotypes. That does not mean one saliva marker explains the whole dog. It does mean the bridge between chronic strain and bodily defense is measurable.
Telomere work adds a more cumulative perspective. In dogs, shorter telomeres have been associated with more chronically adverse or institutional life contexts. Documented That does not license dramatic claims about every excitable home aging its dog prematurely. It does support the broader point that long-duration stress can carry biological cost well beyond visible behavior.
Why It Matters for Your Dog
This Foundation matters because it changes the seriousness with which families interpret chronic dysregulation. Mixed Evidence A dog that is always activated is not only hard to live with. It may also be paying a quieter biological price in immune strain, poor recovery, or accumulated physiological wear.
That is why JB keeps insisting that calmness is protective. Not because every exciting moment is dangerous, and not because every happy household noise becomes disease risk, but because long-term strain is costly in dogs when it becomes chronic enough and deep enough. The safest household approach is therefore one that reduces stacked stress rather than normalizing it.
Calmness matters partly because chronic strain has body costs. The calmer household is not only easier to live in. It is a more biologically conservative environment for the developing dog.
This also helps families think more clearly about illness. A dog who is suddenly more irritable, restless, clingy, or unable to settle may not be showing a "training problem" at all. Sometimes the feedback loop is running from the body back into the behavior, and the humane response is medical curiosity rather than stricter handling.
The practical takeaway is not panic. It is respect. Chronic stress is a whole-animal issue. When the behavior looks persistently dysregulated, the body deserves to be part of the conversation too.
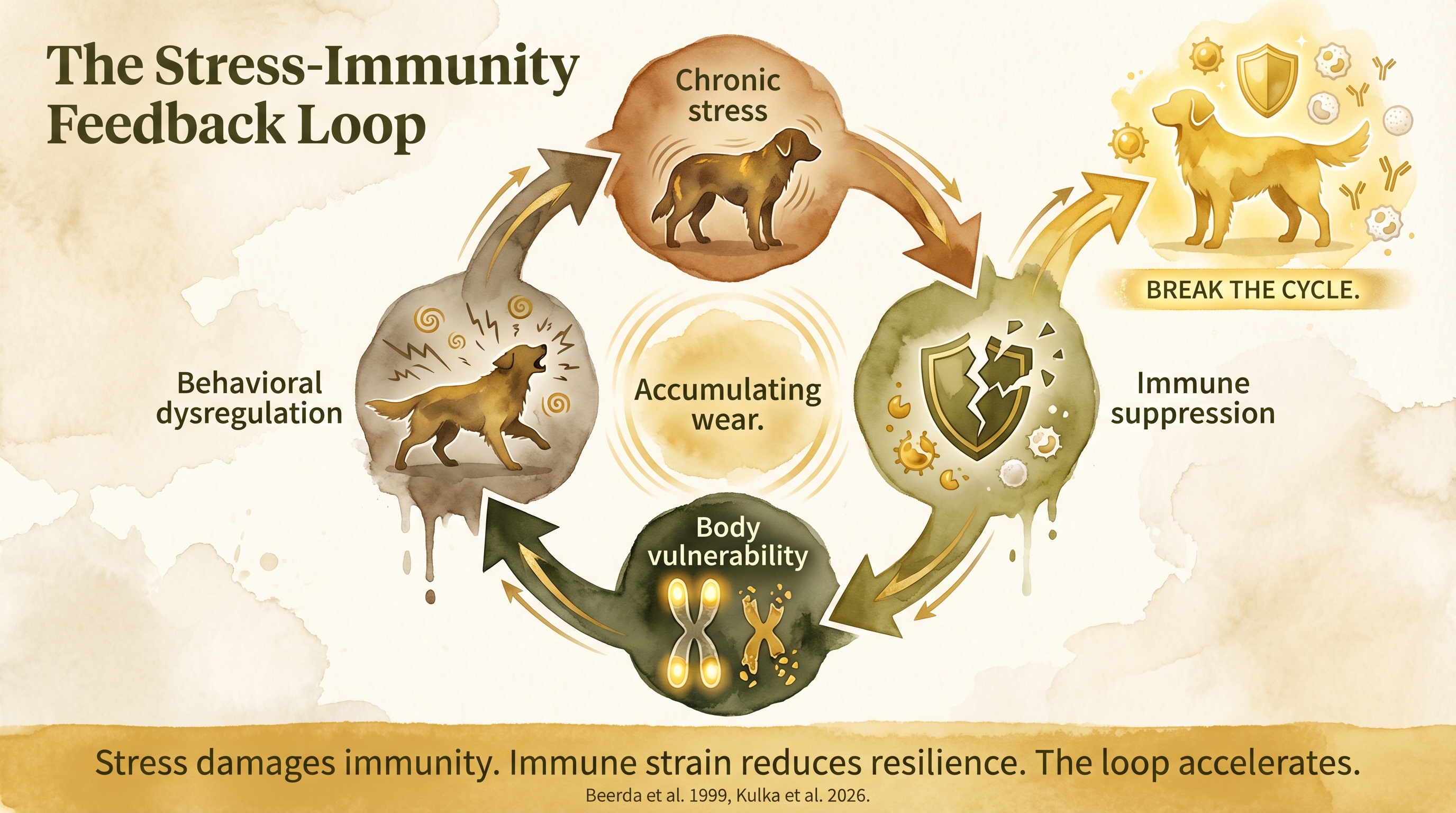
Stress damages immunity, immune strain reduces resilience, and the loop accelerates - chronic stress leaves measurable biological footprints beyond behavior alone.
Key Takeaways
- Chronic stress in dogs can alter immune-related function, which means dysregulation is not only a behavior issue.
- The strongest evidence comes from more adverse long-duration stress contexts, so ordinary household-arousal claims should stay restrained.
- Physical strain can then feed back into behavior by reducing tolerance, disrupting sleep, and making regulation harder.
- Families should treat persistent dysregulation as a whole-animal concern that may require health, environment, and relationship thinking together.
The Evidence
This entry uses mixed-evidence claim-level tags beyond the dedicated EvidenceBlocks below. These tags mark claims that combine documented findings with observed practice, heuristic application, or unresolved gaps.
- Beerda, B. et al. (1999)domestic dogs
Documented hormonal and immunological effects of chronic social and spatial restriction. - Kulka, M. et al. (2026)domestic dogs
Found meaningful stress-related differences in canine lymphocyte expansion, activation, and apoptosis. - Dudley, E. S. et al. (2015)domestic dogs
Shelter dogs showed stress-linked physiologic changes, reinforcing that chronic adverse environment affects more than behavior.
- Skandakumar, S. et al. (1995) and Svobodova, I. et al. (2014)domestic dogs
Linked cortisol with salivary IgA dynamics, showing measurable stress-immune interaction in dogs. - Dutra, L. M. L. et al. (2025)domestic dogs
Associated shorter telomeres with more adverse or institutional canine life contexts, showing a possible cumulative biological cost of long-duration stress.
- Stress-type boundary synthesisdomestic dogs
The strongest documented dog evidence concerns chronic adverse environments, so the stronger claim that ordinary household excitability alone produces the same biological costs remains more interpretive.
No published study has measured whether lowering ordinary household stimulation changes immune markers or long-term biological stress burden in family-raised dogs.
The field still lacks longitudinal puppy-to-adult work tracing how chronic dysregulation, illness burden, and behavior interact across years in the same dogs.
SCR References
Sources
Beerda, B., et al. (1999). Chronic stress in dogs subjected to social and spatial restriction. II. Hormonal and immunological responses. Physiology & Behavior.
Dudley, E. S., et al. (2015). Effects of repeated petting sessions on leukocyte counts, parasite prevalence, and plasma cortisol concentration of dogs housed in a county animal shelter. JAVMA.
Dutra, L. M. L., et al. (2025). Telomere Tales: Exploring the impact of stress, sociality, and exercise on dogs cellular aging. Veterinary Sciences.
Kulka, M., et al. (2026). Stress-related immunomodulation of canine lymphocyte responses and hematologic profiles. International Journal of Molecular Sciences.
Skandakumar, S., et al. (1995). Salivary IgA: A possible stress marker in dogs. Animal Welfare.
Svobodova, I., et al. (2014). Cortisol and secretory immunoglobulin A response to stress in German Shepherd dogs. PLOS ONE.