Taurine in Canine Diets
Taurine is one of the most misunderstood nutrients in the modern dog-food conversation because it sits at the intersection of real biochemistry, breed-specific concern, and a much larger unresolved debate about diet-associated dilated cardiomyopathy. Families often hear one of two bad simplifications: dogs do not need taurine, so it does not matter, or taurine explains the whole grain-free DCM story. Neither statement is good enough. Taurine matters greatly in dogs, especially in cardiac biology, but the way it matters is species-specific, breed-sensitive, and more conditional than many families first realize. Documented
What It Means
Taurine is a sulfur-containing amino acid-like compound involved in bile acid conjugation, cell membrane stability, osmoregulation, retinal and neurologic function, and most importantly for this page, cardiac muscle function. It helps explain why taurine deficiency can produce such serious consequences when it does occur. The heart is not peripheral to taurine biology. It is one of the main reasons the molecule matters clinically.
The dog-cat distinction is the first thing families need to know. Cats have an absolute dietary taurine requirement because they cannot synthesize enough on their own. Dogs are different. Dogs can usually synthesize taurine from methionine and cysteine, the sulfur amino acids supplied by dietary protein. That is why taurine is not treated as absolutely essential in standard canine nutrient tables in the same way it is for cats.
That difference sometimes gets turned into a false comfort statement: dogs make taurine, so taurine is not a real issue. The better reading is that most dogs can maintain taurine status under ordinary conditions, but not all dogs under all diet patterns do so equally well.
Why Breed Matters
Golden Retrievers are central to this conversation because they are one of the breeds in which taurine-deficient, diet-associated DCM has been documented. Cocker Spaniels and Newfoundlands also appear in the taurine-sensitive literature. This does not mean every dog in those breeds is metabolically doomed. It means the breed pattern is strong enough that clinicians cannot dismiss taurine when these dogs present with compatible diet history and cardiac disease.
The most responsible sentence is that some breeds appear to have lower margin for error around taurine homeostasis, whether because of synthesis efficiency, requirement differences, diet interaction, or other host factors still not fully resolved. Golden Retrievers sit inside that higher-concern group.
How Diet Can Interact With Taurine Status
Taurine status is not determined only by how much taurine is listed on a label. Dogs synthesize taurine from methionine and cysteine, so precursor supply matters. Digestibility matters. Bile acid handling matters. Fiber burden matters. The broader matrix of the diet matters.
This is why lamb-and-rice diets entered earlier taurine discussions, and why later pulse-heavy, grain-free diets drew so much attention. Some diet patterns may reduce sulfur amino acid availability, increase fecal loss of taurine-conjugated bile acids, or otherwise create a metabolic environment in which susceptible dogs struggle to maintain taurine status. Documented This is a more nuanced picture than "grain-free equals low taurine," but it still makes diet composition highly relevant.
The pulse question matters here. Peas, lentils, and chickpeas are not evil ingredients by definition, but heavy inclusion of these components in certain formulas has been part of the working hypothesis for diet-associated DCM because of their possible effects on precursor availability, digestibility, and bile acid dynamics. Documented This remains an active area of uncertainty rather than a solved mechanism, but it is one reason taurine cannot be discussed as though it lives independently from the rest of the formula.
Taurine and the DCM Conversation
The strongest documented taurine story is the Golden Retriever DCM subset. Kaplan and related literature showed affected Goldens with low taurine and cardiomyopathy improving after diet change plus supplementation. That is not an internet rumor. It is a real clinical pattern.
The broader diet-associated DCM literature then complicated the story by showing that not every affected dog is taurine deficient. Some dogs with suspect diet histories had normal taurine concentrations. That means taurine deficiency explains some diet-associated cardiac cases but not all of them. The broader grain-free and BEG debate therefore cannot be collapsed entirely into one amino acid.
This is exactly why SCR-077 and SCR-078 belong together. SCR-077 says taurine-deficient, diet-associated DCM is documented in Goldens. Documented SCR-078 says the blanket claim that grain-free diets cause DCM is too strong. Both statements are true at once.
How Taurine Is Tested
When taurine deficiency is suspected, whole blood taurine is generally the preferred sample because it reflects tissue status more robustly than plasma alone. Plasma taurine can still be useful, especially when whole blood is not available, but whole blood is typically treated as the stronger test in clinical interpretation.
Testing matters because casual supplementation before sampling can blur the picture. Families who strongly suspect the issue often want to start taurine immediately, which is understandable. But if the dog is stable enough and a diagnostic workup is underway, clinicians may prefer to collect samples first. If the dog is symptomatic or already under cardiology care, treatment decisions may move quickly in parallel with testing.
How Taurine Is Managed
Management usually includes both supplementation and diet change. Observed-JB Taurine supplementation alone is not the whole answer when the diet pattern itself is under suspicion. In a Golden Retriever-sized dog, typical clinical taurine dosing often falls around 500 to 1000 mg twice daily, though the exact plan belongs to the treating veterinarian or cardiologist.
Echocardiographic monitoring matters because the goal is not just to normalize a number on paper. The goal is to know whether cardiac structure and function are improving, stabilizing, or worsening. Taurine in this context is part of a cardiac management pathway, not just a nutrient add-on.
Why It Matters for Your Dog
This page matters because taurine is where families can easily swing into either neglect or overreaction. Some hear that dogs synthesize taurine and stop caring about it. Others hear one Golden story and assume every grain-free food is silently draining taurine from every dog. Neither response helps.
For your dog, the practical value of this page is twofold. First, it explains why Goldens deserve more respect in this area than the generic dog population average might suggest. Second, it explains why taurine questions belong inside a fuller diet and cardiac context rather than being treated as a one-pill fix.
The safest use of taurine science in Goldens is not to hope supplementation rescues a bad feeding plan later. It is to avoid creating the risky diet pattern in the first place unless a veterinarian has a compelling medical reason to choose it.
This page also matters because it helps families ask much better questions when the issue surfaces. Instead of saying "does this food have taurine," the more useful questions are: what is the dog's breed risk, what is the diet pattern, are pulses or unusual ingredient structures prominent, is the dog symptomatic, and should taurine and cardiac status be evaluated together. Documented
Another practical reason this matters is that taurine does not excuse weak formulation. Some families imagine they can keep feeding a questionable diet as long as they add taurine. That may not solve the real problem if the broader diet pattern is still contributing to disease risk through mechanisms not fully captured by taurine numbers alone.
Finally, this page matters because it teaches evidence humility. Taurine is one of the clearest documented pieces of the diet-associated DCM story in Goldens, but it is not the whole story. That makes it important, not magical.
It is also worth understanding why taurine sits at the meeting point of protein, fiber, and bile acid biology. Dogs synthesize taurine from methionine and cysteine, so diets low in sulfur amino acid availability or lower in usable protein quality can reduce the margin for comfortable synthesis. At the same time, taurine is used to conjugate bile acids, which means changes in bile acid recycling and fecal loss can change taurine economy inside the body. This is one reason pulse-heavy, higher-fiber, and otherwise nontraditional formulations remain mechanistically interesting even when a label appears to meet crude nutrient minimums.
Earlier taurine literature also reminds families that the problem is not confined to one trendy modern ingredient. Lamb-and-rice diets became part of taurine history because some dogs on those patterns developed deficiency-related concerns long before the grain-free era took over public attention. That older history matters because it keeps the family from telling too simple a story. Taurine vulnerability is about diet pattern and host response, not about one slogan-friendly villain alone.
Testing nuance matters too. Plasma taurine can fluctuate more with recent intake and short-term status, whereas whole blood taurine tends to reflect body stores more robustly. Families do not need to become laboratory specialists, but they should understand why a cardiologist or internist may care about which sample is drawn and when. In a suspected diet-associated cardiac case, taurine measurement is one piece of a coordinated workup rather than a standalone screening novelty.
Supplementation also needs context. Taurine is often used generously because safety margins are relatively good, but dose choice, duration, and follow-up still belong to the veterinarian. Some dogs improve dramatically. Some improve partly. Some show that the diet-related concern was broader than taurine alone. That is why repeat cardiac imaging is so important. The dog is not being treated to make the bloodwork prettier. The dog is being treated to improve or stabilize heart function.
For Golden families, the practical synthesis is therefore very straightforward. Taurine science is strong enough to justify caution with nontraditional diets and to justify real diagnostic seriousness when cardiac signs appear. It is not strong enough to justify the claim that every Golden needs routine taurine supplementation forever regardless of diet. The evidence lives in the middle: respect the breed signal, respect the diet pattern, and use taurine intelligently rather than superstitiously.
Another useful practical point is that taurine response is often part of a package rather than a single-variable story. Dogs in the published Golden literature often improved after diet change, taurine supplementation, and standard cardiac therapy together. Families should hear that carefully. The improvement pattern is clinically encouraging, but it also means taurine should be understood as one major tool inside a coordinated cardiac plan, not as a stand-alone rescue myth.
That is why cardiology follow-up matters so much. If taurine deficiency is suspected, clinicians are not only trying to normalize a lab result. They are watching whether systolic function improves, whether chamber dimensions stabilize, whether arrhythmia burden changes, and whether the dog's exercise tolerance returns. The bigger lesson is that taurine is important precisely because it is tied to meaningful heart outcomes, not because it is a fashionable supplement category.
Families also deserve the reassurance that this topic has a rational default. Most dogs eating well-formulated mainstream diets do not need families to become taurine hobbyists. Taurine becomes a priority when breed signal, diet pattern, and clinical context make it relevant. That is why the most adult approach is neither fear nor dismissal. It is appropriate seriousness when the case truly calls for it.
That calm default is one of the best protections against both panic and fad supplementation.
It keeps the family focused on the dogs who actually need taurine-centered attention most.
That focus is what makes the topic clinically useful instead of merely fashionable.
When to See a Veterinarian
Veterinary evaluation is appropriate if a Golden Retriever or other higher-concern breed is eating a nontraditional or pulse-heavy diet and develops exercise intolerance, reduced stamina, cough, fainting, weakness, rapid breathing, or any decline in ordinary activity comfort. These are possible cardiac signs, not just nutrition signs.
Families should also seek veterinary guidance if they are feeding a grain-free or BEG-pattern diet and simply want to know whether taurine testing is appropriate. A veterinarian may recommend taurine measurement, diet change, cardiac screening, or cardiology referral depending on the history and the dog's status.
Urgent evaluation is needed for collapse, labored breathing, severe weakness, or abdominal swelling. Those can reflect advanced cardiac compromise and should not wait on nutrition debate.
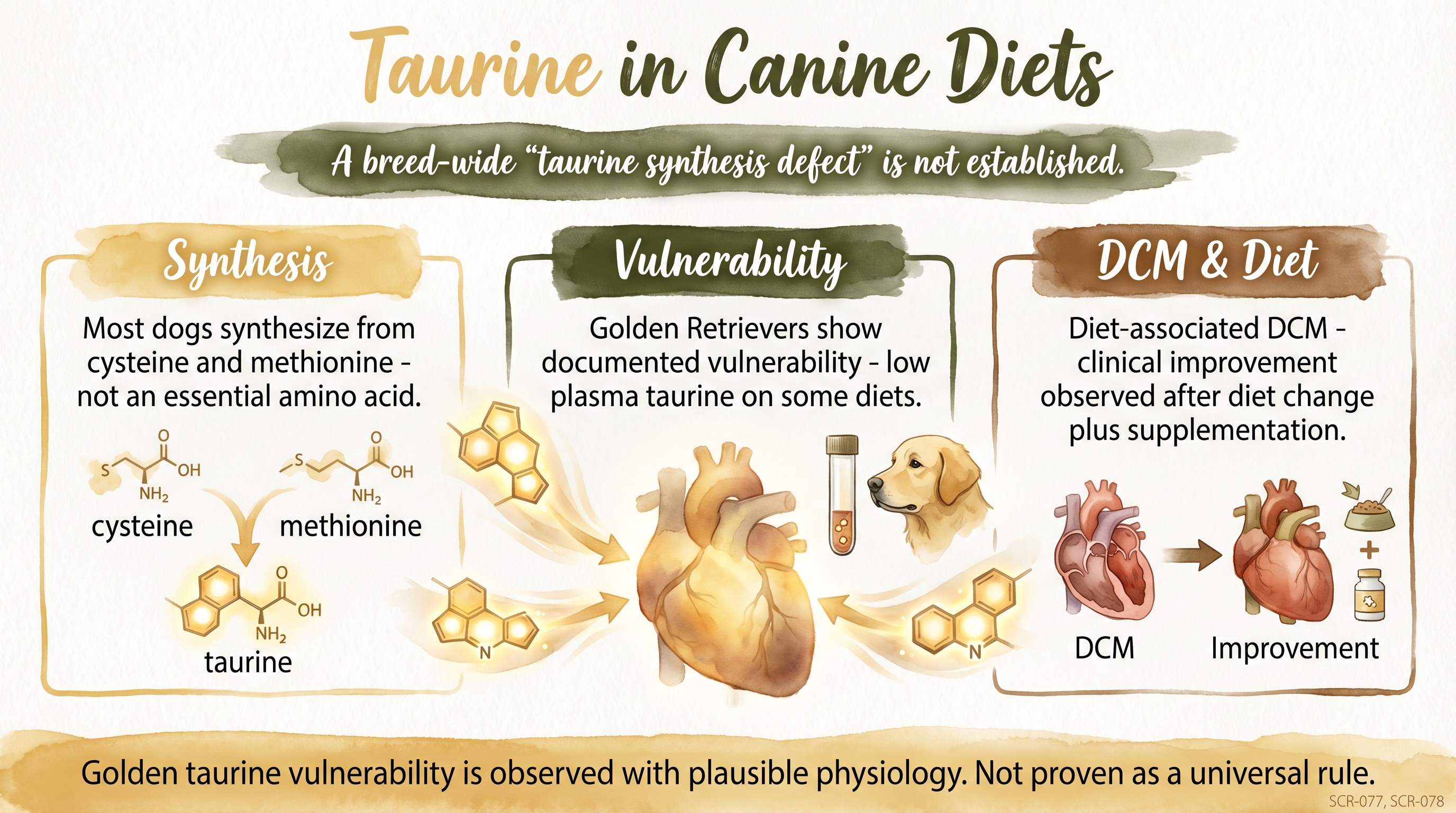
Golden taurine vulnerability is observed with plausible physiology, not proven as a universal rule.
Key Takeaways
- Dogs usually synthesize taurine, but that does not make taurine irrelevant because some breeds and some diet patterns appear to reduce the margin for safety.
- Golden Retrievers are one of the clearest breeds in the documented taurine-deficient, diet-associated DCM literature.
- Whole blood taurine is generally the preferred clinical test when deficiency is being evaluated.
- Taurine supplementation can help some affected dogs, but it should not be treated as a substitute for correcting a suspect diet pattern or for proper cardiac evaluation.
The Evidence
This entry uses observed claim-level tags beyond the dedicated EvidenceBlocks below. These tags mark JB program observation or practice-derived claims that need dedicated EvidenceBlock coverage in a later content pass.
The core documented statement is SCR-077: taurine-deficient, diet-associated DCM exists in Golden Retrievers and some affected dogs improve with diet change plus taurine supplementation and standard cardiac therapy. The major boundary is SCR-078: the larger grain-free and BEG issue is still multifactorial and unresolved, so taurine is central but not exhaustive.
That is the right family-level conclusion too. Taurine deserves to be taken seriously in Goldens. It does not deserve to be treated as a total explanation for every diet-associated cardiac concern.
- SCR-077 supportGolden Retrievers
Taurine-deficient, diet-associated DCM is documented in Goldens, with meaningful improvement reported in some dogs after diet change and taurine supplementation. - Golden and breed-sensitive taurine literaturedogs
Certain breeds, including Golden Retrievers, appear more vulnerable to taurine-related cardiac compromise than the average dog population. - Clinical taurine testing frameworkdogs
Whole blood taurine is generally preferred over plasma alone when deficiency is being evaluated clinically.
- SCR-078 boundarydogs
The blanket claim that grain-free diets cause DCM remains too strong because not all affected dogs are taurine deficient and the mechanism is not fully resolved. - Diet-pattern interaction literaturedogs
Pulse-heavy and nontraditional diets remain clinically relevant because taurine status depends on broader precursor supply, digestibility, and bile-acid handling rather than on taurine as an isolated label feature.
No published study directly tests the practical implications of taurine in canine diets for domestic dog raising programs. The application to household dog raising remains an interpretive synthesis rather than a directly tested intervention finding.
SCR References
Sources
- National Research Council. (2006). Nutrient Requirements of Dogs and Cats. Washington, DC: The National Academies Press.
- AAFCO. (2024). Official Publication. Association of American Feed Control Officials.
- Kaplan, J. L., Stern, J. A., Fascetti, A. J., Larsen, J. A., Skolnik, H., Peddle, G. D., Kienle, R. D., Waxman, A., Cocchiaro, M., Gunther-Harrington, C. T., Klose, T., LaFauci, K., Lefbom, B., Machen Lamy, M., Malakoff, R., Nishimura, S., Oldach, M., Rosenthal, S., Stauthammer, C., ... Yu, S. (2018). Taurine deficiency and dilated cardiomyopathy in Golden Retrievers fed commercial diets. PLOS ONE, 13(12), e0209112.
- Freeman, L. M., Stern, J. A., Fries, R., Adin, D. B., & Rush, J. E. (2018). Diet-associated dilated cardiomyopathy in dogs: what do we know? Journal of the American Veterinary Medical Association, 253(11), 1390-1394.
- Adin, D., DeFrancesco, T. C., Keene, B., Tou, S., Meurs, K., Atkins, C., Aona, B., Kurber, K., Reimer, S., & Sederquist, K. (2019). Echocardiographic phenotype of canine dilated cardiomyopathy differs based on diet type. Journal of Veterinary Cardiology, 21, 1-9.