Pancreatitis in Dogs
Compound evidence detail1 SCR / 3 parts
- Documentedthe diagnostic combination of clinical signs, Spec cPL or cPLI testing, and abdominal imaging - with serum amylase and lipase alone insufficient - alongside the supportive-care treatment standard of intravenous fluid therapy, analgesia, antiemetics, and early enteral nutrition
- Documentedthe role of obesity, dietary indiscretion, endocrinopathies, and breed factors as documented contributors to canine pancreatitis risk, with weight management and fat-restricted diets as recurrence-reduction levers in predisposed dogs
- Heuristicthe dietary fat percentage recommended after pancreatitis recovery - consensus-derived from clinical practice rather than established by outcome-validated trial data
Pancreatitis is one of those diagnoses that families often hear after a dog seems to have "just a stomach bug" that turns out to be more serious than expected. The pancreas is a small organ with outsized importance. When it becomes inflamed, dogs can swing from mild nausea and vomiting to severe abdominal pain, dehydration, and hospitalization needs. The right family posture is not panic at every vomit. It is respect for the signs that suggest this is not ordinary transient GI upset anymore. Mixed Evidence
What It Means
What Pancreatitis Is
Pancreatitis is inflammation of the pancreas. In the broadest sense, the problem is that digestive enzymes and inflammatory pathways become activated in a way that injures pancreatic tissue and affects the rest of the body.
Dogs may experience acute pancreatitis; chronic pancreatitis; and recurrent low-grade episodes that only become obvious over time. Mixed Evidence
The clinical picture varies widely, which is why this page needs both caution and proportion.
Acute Versus Chronic
Acute pancreatitis is the version families usually notice most clearly. The dog is suddenly vomiting, painful, lethargic, and not acting normal. Some dogs assume a hunched posture or become reluctant to move because the abdomen hurts.
Chronic pancreatitis is trickier. These dogs may have intermittent nausea; softer stools; reduced appetite on and off; and repeated smaller GI flares. Mixed Evidence
Over time, recurrent pancreatic inflammation may contribute to broader pancreatic dysfunction, including metabolic and digestive consequences. Documented
What Triggers It
Some cases follow an obvious trigger. Others do not.
Common associations include high-fat dietary indiscretion, obesity, certain medications, endocrine disease, and idiopathic cases where no clear trigger is found. Documented
Families often focus on the one unusually rich meal because that is the easiest story to remember. Sometimes that story is true. Sometimes it is only the visible last event in a dog who was already metabolically vulnerable.
Why Body Condition Matters
This is one of the places where the broader JB weight-management logic matters. Lean body condition is one of the clearest modifiable health advantages in dogs. While pancreatitis is not reducible to "fat dogs get pancreatitis," excess weight clearly worsens the metabolic terrain in which inflammatory and GI disease plays out.
That is why prevention here does not only mean avoiding table scraps. It also means not normalizing chronic overweight status.
What Families Usually Notice
Typical signs include repeated vomiting, abdominal pain, lethargy, reduced appetite, diarrhea in some cases, reluctance to move, and dehydration.
Some dogs have classic severe signs. Others look simply dull and nauseated. That variability is one reason pancreatitis can be missed early.
Why It Matters for Your Dog
How Diagnosis Works
Diagnosis is usually based on a combination of history and examination; pancreatic lipase testing such as Spec cPL; abdominal ultrasound; bloodwork; and ruling out other causes of vomiting and abdominal pain.
No single test exists in a vacuum. A compatible history plus compatible signs plus supportive testing builds the case.
Treatment
Treatment is supportive and depends on severity. Common components include fluid therapy, anti-nausea medication, pain control, nutritional support, and monitoring for complications.
Older dogma sometimes emphasized prolonged withholding of food. Modern care more often focuses on reintroducing appropriate nutrition once vomiting is controlled and the dog can tolerate it.
This is one of the reasons families should not treat pancreatitis as a home remedy problem when a dog is significantly ill. Severe cases deserve real medical support.
Prognosis
Mild cases may improve quickly with supportive care. Severe cases can be life-threatening. Chronic cases can recur and become a frustrating pattern rather than one isolated event.
The prognosis therefore depends less on the label alone and more on severity; hydration; response to treatment; recurrence pattern; and whether the dog has concurrent disease. Documented
Why This Page Matters for Goldens
Goldens are not the single classic pancreatitis breed, but they are a large family breed in which body condition, dietary indulgence, and general GI issues commonly matter. That makes pancreatitis relevant even if it is not the signature Golden disease in the way cancer is a signature Golden disease.
This page also matters because it helps families distinguish ordinary brief GI upset; pancreatitis-level concern; and chronic GI patterns that need deeper workup.
When to See a Veterinarian
Veterinary evaluation is warranted for repeated vomiting, obvious abdominal pain, lethargy with GI signs, inability to keep water down, worsening weakness, and recurrence after a known dietary indiscretion.
Same-day evaluation is especially appropriate when vomiting is persistent, the dog looks painful, or the dog is becoming weak or dehydrated.
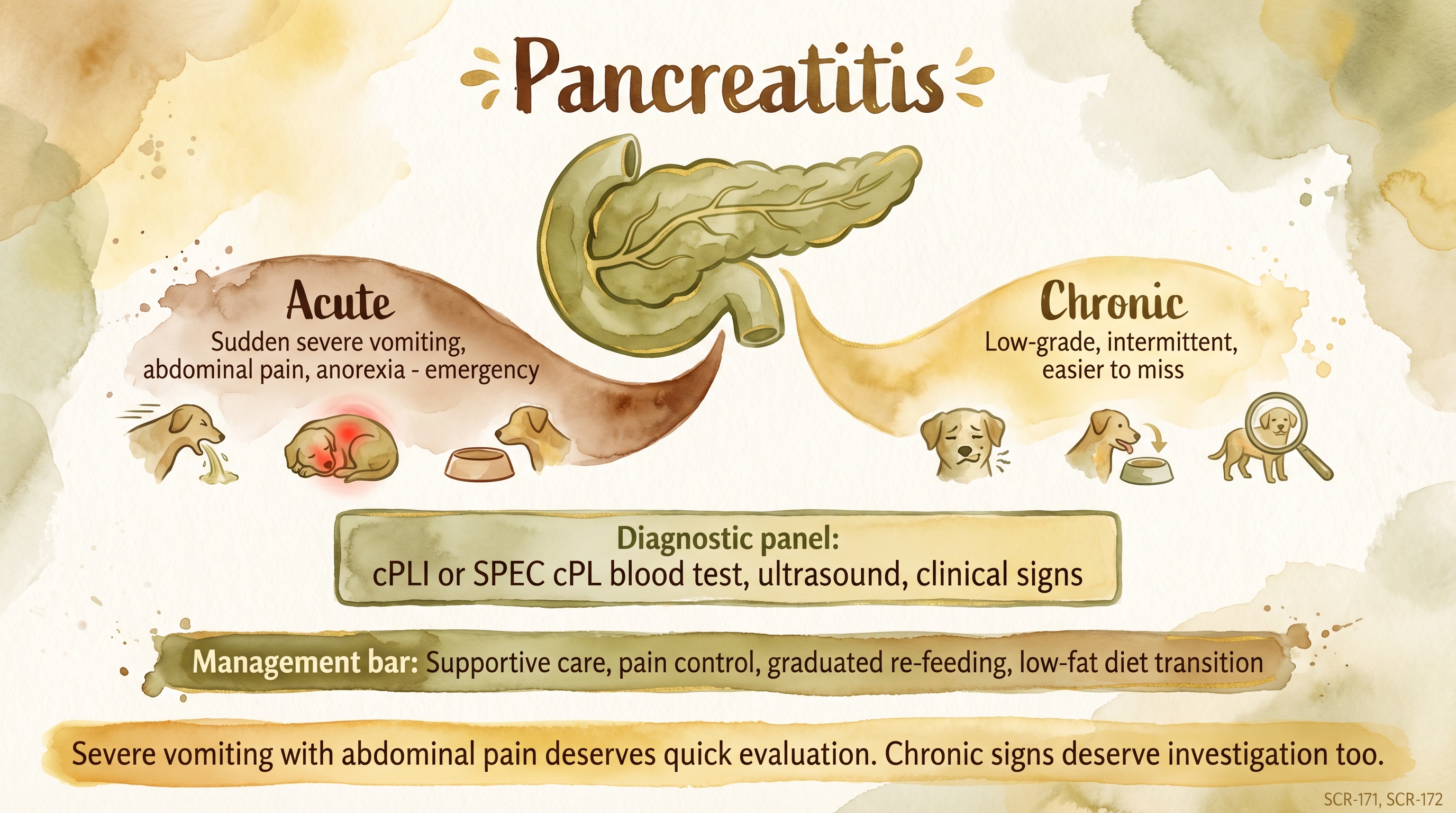
Severe vomiting with abdominal pain deserves quick evaluation - chronic signs deserve investigation too.
Key Takeaways
- Pancreatitis ranges from mild nausea and vomiting to severe painful illness requiring hospitalization.
- Acute and chronic forms both matter, and some dogs declare themselves through recurrent smaller flares rather than one huge crisis.
- Diagnosis depends on the whole clinical picture, not one isolated number or one isolated meal history.
- Repeated vomiting, abdominal pain, weakness, or inability to keep water down are the practical signs families should take seriously right away.
The Evidence
This entry uses mixed-evidence claim-level tags beyond the dedicated EvidenceBlocks below. These tags mark claims that combine documented findings with observed practice, heuristic application, or unresolved gaps.
- ACVIM and internal-medicine literaturedogs
Canine pancreatitis spans acute and chronic presentations and is diagnosed using compatible clinical signs, pancreatic lipase testing, imaging, and exclusion of differentials. - Supportive-care literaturedogs
Treatment is largely supportive, centered on fluids, analgesia, antiemetics, and nutritional management rather than one curative drug. - Clinical risk frameworkdogs
Dietary indiscretion and metabolic burden can contribute, but many cases remain idiopathic and should not be reduced to one simplistic trigger.
- SCR-075 supportdogs
Lean body condition remains one of the strongest modifiable health advantages in dogs and is part of the preventive logic around many chronic inflammatory conditions. - Diet-disease source synthesisdogs
Chronic overconditioning meaningfully worsens the physiologic terrain in which pancreatic and GI disease unfolds.
- domestic dogs
No published study directly compares the most effective long-term management paths for pancreatitis in dogs in dogs across breeds and ordinary home settings.
SCR References
Sources
- Xenoulis, P. G. (2015). Diagnosis of pancreatitis in dogs and cats. Journal of Small Animal Practice, 56(1), 13-26. https://doi.org/10.1111/jsap.12274
- Mansfield, C. (2012). Acute pancreatitis in dogs: Advances in understanding, diagnostics, and treatment. Topics in Companion Animal Medicine, 27(3), 123-132. https://doi.org/10.1053/j.tcam.2012.04.003
- World Small Animal Veterinary Association. (n.d.). Global nutrition guidelines. https://wsava.org/global-guidelines/global-nutrition-guidelines/
- Kealy, R. D., Lawler, D. F., Ballam, J. M., Mantz, S. L., Biery, D. N., Greeley, E. H., Lust, G., Segre, M., Smith, G. K., & Stowe, H. D. (2002). Effects of diet restriction on life span and age-related changes in dogs. Journal of the American Veterinary Medical Association, 220(9), 1315-1320. https://doi.org/10.2460/javma.2002.220.1315
- Boundary approved by Queue1-DecisionTree: the existing Xenoulis (2015) and Mansfield (2012) citations support a narrower canine pancreatitis diagnosis and supportive-care boundary. SCR-075 is now Verified but supports lifespan / body-condition context, not pancreatitis itself. SCR-186 remains Pending PSV for the full pancreatitis claim package.